In 2014 East Surrey clinical commissioning group (CCG) embarked on a project to improve the medical care of residents of nursing and residential homes (care homes). East Surrey CCG has a significant number of Care Homes with a total of 1,800 beds across the geography. This example of a local initiative forms part of our managing transfers of care resource.
There are 20 care homes with nursing (nursing homes) in East Surrey CCG and over a 100 care homes providing personal care (residential homes). Today, care homes with nursing and/or personal care manage residents with more complex health needs than in the past as well as providing more end of life care, allowing residents to achieve their Preferred Place of Care (PPC) at the end of their lives.
Both national and local evidence shows that GPs felt that the medical care of residents of care homes was unsatisfactory and the lack of support and resources brought into question the quality of the service. This was highlighted in a 2011 King’s Fund workshop (national data):
- 61 per cent of GPs found current arrangements for medical care of patients in care homes unsatisfactory
- 40 per cent - GPs felt medical support for care homes below average or poor
- 70 per cent - GPs felt depression and dementia was not optimally managed.
Within care homes there was a lack of confidence in healthcare provision and a view that out-of-hours would routinely "send to hospital" – with a lack of available information with regards to a plan of care. Care homes also struggle to recruit adequate numbers of staff and staff with appropriate skills or provide the skills and training required. On any one day, there are 90,000 vacancies for social care jobs in England, according to Skills for Care.
Local data also demonstrated that patients are usually unable to attend the primary care centres requiring visits to the care home, frequent and multiple prescribing interventions and they have a higher than average use of out-of-hours Services. The King’s Fund event had found also that:
- 68 per cent of GPs reported that care homes as a major source of stress for GPs
- 73 per cent of GPs – felt there was a lack of support or resources to manage patients in care homes safely.
From geriatricians, key findings were that: 73 per cent wanted greater involvement in care home work. Locally, significant numbers of patients from care homes were dying inappropriately in hospital within 24 hours of admission, rather than their place of choice.
The plan
The key aim was enhancing the level of care to all residents of care homes based on a proactive and preventative approach to care using personal planning and reducing the variation in care experienced across care homes by:
- increasing GP time to support care homes
- care coordinated approach
- improved medicine management support and training
The project was designed to be developed and embedded over a period of time with new features being built in once early components had been bedded in and consolidated.
For Phase 1 - the proposed service model was structured around four components:
- Nurse advisors for care homes – First Community Health and Care (Community Provider)
- Redesign of the locally commissioned service (LCS) to facilitate work of GPs in Care homes
- Pharmacy
- New ambulance pathway
- Nurse Advisors: Nurse Advisors for care homes were engaged more widely to help deliver improvements. This included protocols to assess the appropriateness of 999 calls and Red/Amber/Green (RAG) rate both nursing and care home. Regular education and upskilling of care home staff with case based discussion was key and performance regularly monitored. The regular involvement of nurse advisors was vital to the success of the project, including by providing support, advise and facilitating training to care home staff to enable the staff to be competent and confident in the management of their residents care to help prevent inappropriate hospital admissions.
- Redesign of LCS: The LCS has given GPs the investment needed to release time to focus on the management of care home patients. Each home now has a named GP so that there is a consistent approach and timeline to patient care. Assessments of new and initial assessments of existing patients are carried out with on-going regular follow-up reviews for all patients. These cover past medical history and currently prescribed medication – (polypharmacy) – to confirm that the medication is appropriate and consider stopping medicines that might, for example, increase risk of falls and latrogenic illnesses.
GPs lead the work to write a care plan for each patient to act as a personalised action plan. Plans are written with the involvement and support of the patient, their family and care home staff. Through Share My Care (SMC) GP out-of-hours electronic system, care plans can be seen by community service providers as well as the out of hours provider.
- Pharmacy: A named pharmacist from the CCG’s Medicine Management Team carries out a thorough review of prescribed medication for each patient and discusses recommended changes with the relevant GP. The pharmacists also delivered structured training to Care Home staff on the handling of medicines and a dietician from the community care provider also presented. Medication waste in care homes has also been addressed with significant consequent savings.
- New ambulance pathway: As the service most likely to attend a patient in an emergency, the involvement of paramedics was critical. The Ambulance Service’s Intelligence Based Information System (IBIS) is designed to enable paramedics to have up-to-date information about a patient's health and their care plans. It is accessed in the call centre and used to direct the attending crews’ response. It has also allowed paramedics to play an integral part in the proactive management and ongoing care of patients; Hear and Treat / See and Treat approach.
Phase 2 sought to develop the work in phase 1 by:
- introducing IBIS/Anticipatory Care Record to secondary care, ambulatory care, frailty unit, integrated reablement unit and emergency department.
- increasing pharmacy support to regularly review more Care Home patients - 1,800 patients - with average length of stay of approximately 20 months.
- enabling access by ambulance service to Directory of Services and promote access to community services, ambulatory care and frailty unit.
- appointing to a dietician post to complement the provision of medicine management.
Phase 3
This phase will consist of developing and commissioning a single enhanced GP provision to cover all homes, to replace the current individual GP practice cover arrangements with homes. Work is underway to explore what this model could look like.
Implementation
As described, the project was designed to be developed and embedded over a period of time with new features being built in once early components had been bedded in and consolidated. Implementation of this project commenced in 2014 and has been clinically led at every stage.
Outcomes
Development of a care homes multi-disciplinary team has seen the following benefits:
- improved quality of patient care as GPs are resourced to increase the support they provide to their care homes’ patients
- improvement in care home’ staffing skills and knowledge
- more appropriate prescribing and reduction in polypharmacy
- improved end-of-life care
- high proportion dying in their preferred place of death
- effective multi-disciplinary approach to care homes’ work in East Surrey
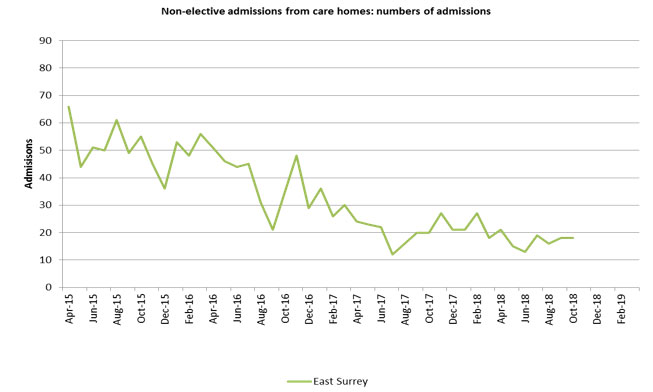
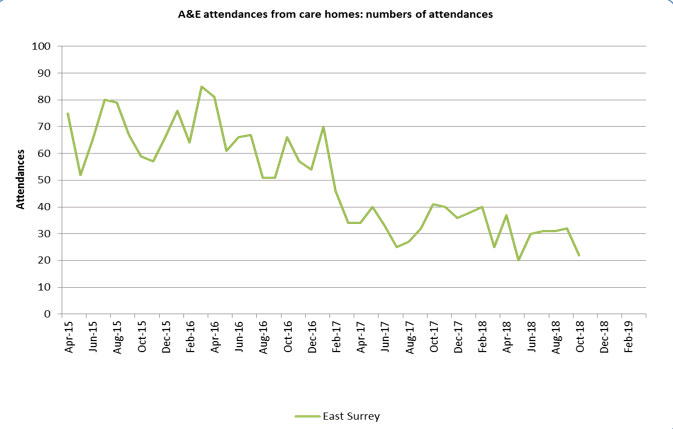
- reduction in unplanned activity from care homes including conveyances, A&E attendances and non-elective admissions.
These benefits have been evaluated and can be quantified as follows:
- 53 per cent reduction in medication waste
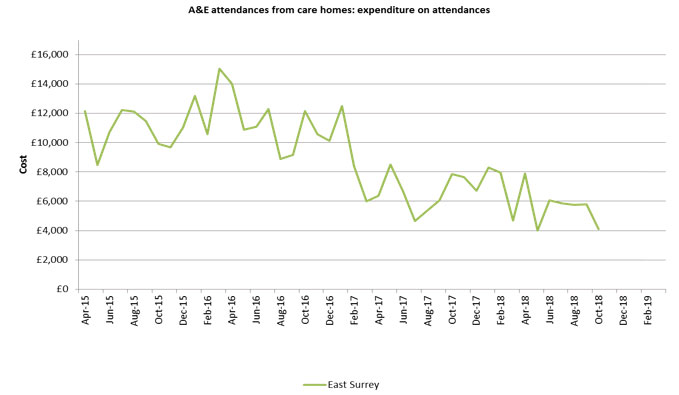
- between September 2015 and December 2018 estimated savings of £200,679 from medicine optimisation
- December 2018 shows a 63 per cent reduction in A&E attendances when compared to 2015
- December 2018 shows a 70 per cent reduction emergency admissions when compared to 2015
- 85 per cent of care home patients dying in care homes as preferred place of death.
Activity reductions and associated cost reductions are demonstrated on the following charts:
Contact
Rebecca Matthews
Lead Manager – Care Homes
[email protected]