Homerton University Hospital’s movement towards seven-day working to improve patient flow has been a long journey that has taken a few of years and gone through a number of iterations in terms of changes to systems and processes. This example of a local initiative forms part of our managing transfers of care resource.
Homerton University Hospital is based in the London Borough of Hackney. The over 18 population is 195,000, with 52 per cent of residents under 20 and only 13 per cent over 55. Hackney is the fifth most deprived borough in the country.
Homerton University Hospital’s movement towards seven-day working to improve patient flow has been a long journey that has taken a few of years and gone through a number of iterations in terms of changes to systems and processes. The hospital started from a position where they had a system of suboptimal processes and interactions between teams and organisations.
The plan
The journey for Homerton Hospital began in 2014 when a number of system changes were introduced around Therapy at Home, a discharge team and a pilot of a full liaison psychiatrist in the Emergency Department.
This then developed into a wider Integrated Intermediate Care and Discharge Service, which included a pilot of an Ambulatory Unit, as well as Geriatrician at the “front door”. Alongside the Geriatrician they introduced a Rapid Access Advice Phone for GPs to provide additional support. Homerton Psychological Medicine was also brought in as part of the integrated service to liaise with the psychiatry service in the ED that had been piloted the previous year.
By 2016, the ambulatory unit have become a fully operational service and Age UK had started a Take Home and Settler Service. All of these developments were supported by the introduction of a number of processes, including improved weekly reporting of wards, specialist and consultant level data, and an increased focused on encouraging morning discharges.
Implementation
Between 2016 and 2018 there was a greater focus on developing weekend working, for example with the creation of a Weekend Discharge Team made up of a social worker, clinical site manager, and therapy consultant. By 2017 the pilot of a Geriatrician at the “Front Door” had developed into a substantive role that was in place Monday-Friday mornings. Alongside these changes the hospital started a Monday-Friday DToC teleconference, improved the daily whiteboard structure on all medical wards and reviewed multi-agency case notes.
The next stage in the development of weekend working was to have a dedicated Weekend Social Worker and Weekend Discharge Consultant, and the hospital began a pilot into Discharge to Assess. To support this the hospital also enhanced their Out of Hours care support.
Outcomes
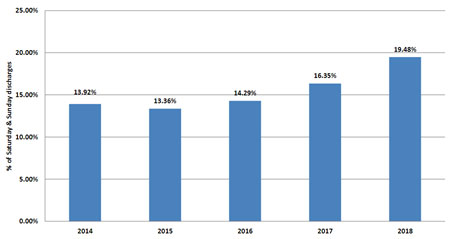
While admissions to the hospital have steadily increased over this period since 2014, Homerton University Hospital has seen median Length of Stay figures fall by almost 50% from their peak in 2015 compared to 2018. In addition, annual DToC bed days have dramatically fallen from a high of 4,145 in 2015/16 to around 2,500 in 2018/19. These reductions have been all within the context of increased seven-day working, which is best illustrated in the table below. From 2015 there has been a steady increase in the percentage of weekend discharges from Acute wards, going from a low of 13.56 per cent in 2015 to 19.48 per cent in 2018.
Despite the successes of moving towards seven-day working, there have been a number of constraints in relation to limited numbers of local care homes and nursing, cancelled and delayed discharges due to transport issues and capacity of the discharge lounge.
Next steps
In terms next steps and where Homerton University Hospital want to develop things further, they are considering a full discharge to assess/home first model, implementing non-medical discharging and further improve referral rates to their Ambulatory Care. They are also looking at moving towards a system of ‘placement without prejudice’ to encourage greater seven-day placements in nursing/care homes.
Contact
Mervyn Freeze
[email protected]