The resource is a practical tool to enable commissioners within councils, housing associations and third-sector organisations to understand the implications of the Digital Switchover for Care Technology and to provide guidance and signposting to where and when action is required. It was developed by the Care and Health Improvement Programme in partnership with Rethink Partners and councils.
Introduction
The resource is intended to cater for a range of approaches - whether the ambition is to safely move telecare users and suppliers on a like-for-like basis from analogue to digital technology or if the ambition is to take this ‘one-off’ opportunity to deliver a more transformational approach to care technology to unlock greater value and be a key driver in changing the operating model for social care, enabling better decisions about people using data and insight.
What is the Digital Switchover and what does it mean for commissioners?
By 2025, analogue telephone services will be switched off as the UK’s telecoms infrastructure is upgraded to digital connectivity. This shift has urgent implications for the digital care technology sector and the millions of people who rely on telecare in the UK.
The transition has begun already with many telecom exchanges having converted over to fully digital. This is starting to affect functionality and connectivity today, and the risk increases from 2023 when BT will no longer sell analogue devices. Action and careful planning needs to begin now so that telecare and social alarm service reliability and safety is not compromised, and that lives are not put at risk. Many in the sector have already started the process, but there are lots of factors for commissioners to consider, and awareness of what it means and what to do varies.
The switchover presents both challenges and opportunities; for example, digital services and equipment are likely to cost more than analogue, which could have a significant impact upon commissioners’ budgets. However, there is also the chance to transform services which could potentially improve services and lower care costs in the longer term.
What do we mean by care technology?
Care technology involves the provision of services such as telecare (long distance monitoring of people to support them to live independently at home), assistive technology and telehealth which provides arrangements for people to manage short and long-term conditions. It can also include the use of newer technologies including video phones, data tools, self-help apps, passive monitoring technology, real-time dashboards and the wider ‘Internet of Things’ that put people in control of their own health, wellbeing and support. There is increasing interest in the data opportunity created by digital technology.
We have learnt in developing this resource that language in this area can be confused; people may use the same terms but mean different things. In this resource, we therefore use the term 'care technology' as a broader umbrella term that captures the increasing complexity and blurred lines between telecare, telehealth, assistive technology, smart equipment, consumer technology, software and smart devices.
What key things do commissioners need to think about?
- Higher costs of digital services and equipment, and the higher ongoing costs of SIM cards, maintenance and upgrades
- Reliability of analogue, hybrid and digital care technology before, during and after the switchover, to ensure the safety of service users
- Capability and quality of suppliers to manage the switchover tasks, communicate with service users, operate and test Alarm Receiving Centres (ARCs) and ensure high standards of cybersecurity
- Procurement and contractual approaches to the switchover which focus on better outcomes for service users, potential transformative benefits and long-term scalability to accommodate much higher numbers of service users
- The significant impact upon service users of the switchover, whether a like-for-like approach is taken or service improvements that digitise more elements of the service
- The opportunities for service redesign or improvement that come with the switchover
What does the digital care technology landscape look like?
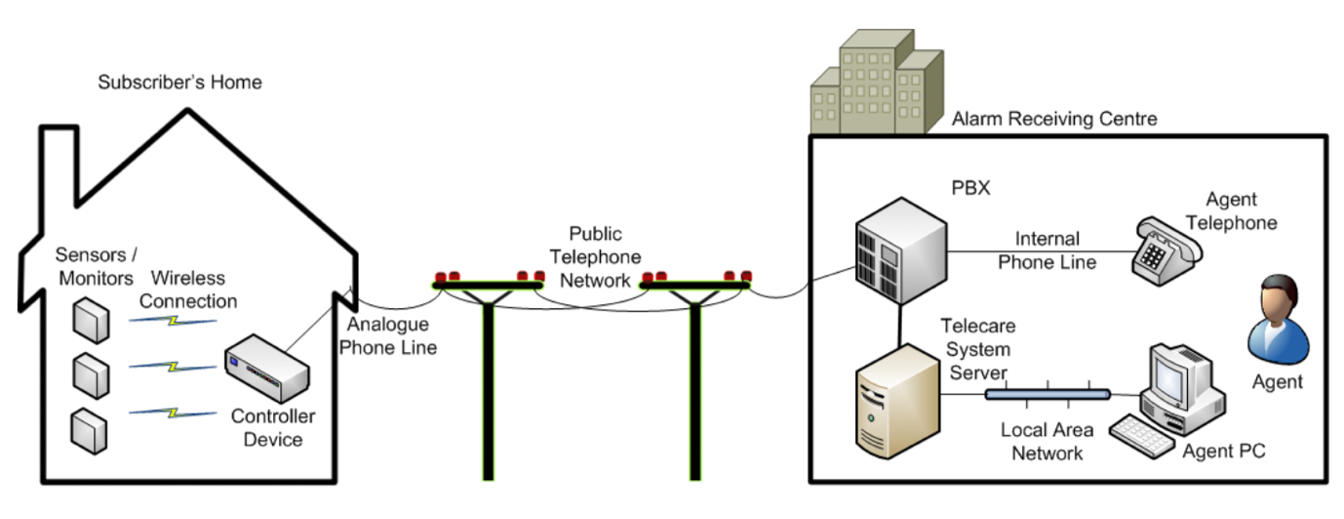
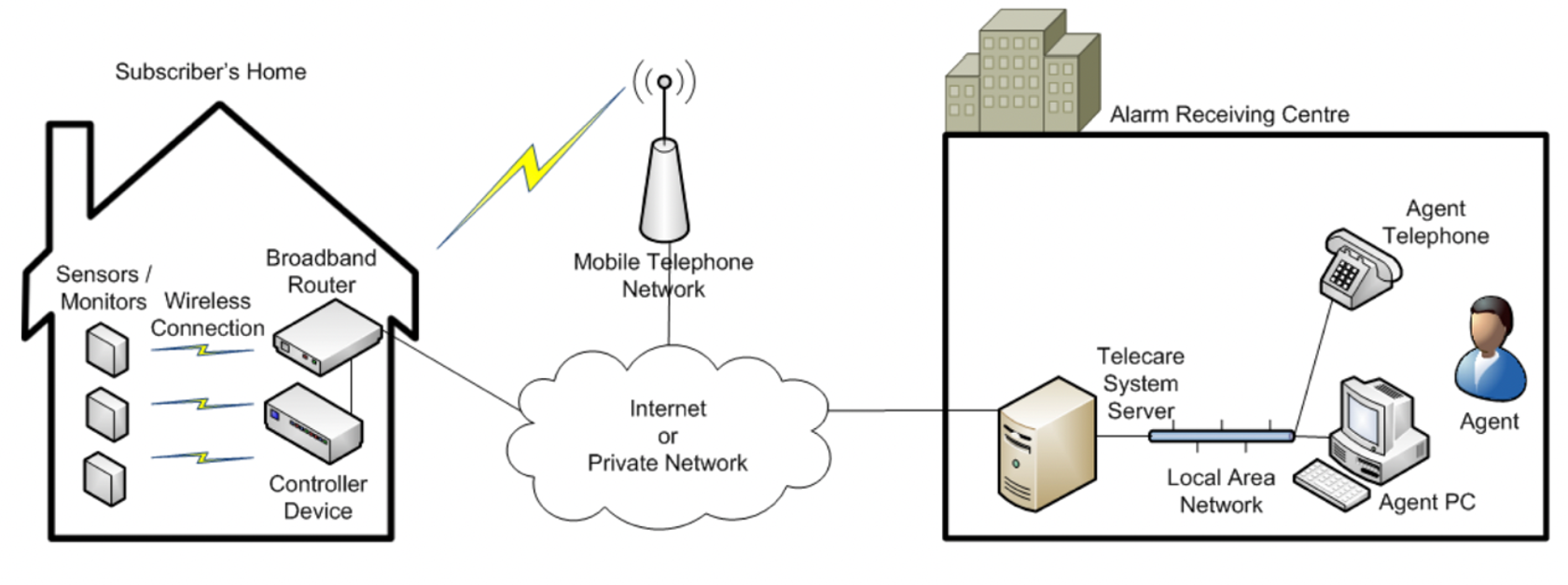
What is the difference between analogue and digital telecare?
Toolkit overview
Step One: Planning
The Digital Switchover is happening already; however, the key dates are 2023 when no new analogue lines and equipment can be purchased from OpenReach; and 2025 when the analogue services will be switched off. With supplier contracts often lasting 5 years or more, commissioners need to be planning how their existing and new contracts cater for this major change in technology.
Step Two: Switchover
The switchover from analogue to digital services may be planned for and organised by technology suppliers, but the impact is likely to be felt most by end-users of the technology when things don’t go smoothly. Commissioners need to consider this impact when procuring, organising and managing services, and may need to put transition support in place.
Step Three: Transformation
Strategically, the switchover to digital technologies offers a ‘one-time’ opportunity to reconsider the way in which care technology and similar services are delivered. Commissioners could plan for simply a ‘like-for-like’ service or take the opportunity for innovation, improved and broadened services and the chance to save money going forward.
- Planning: Readiness assessment
- Switchover: Checklist
- Transformation: Business case
- Planning: Resources
- Switchover: resources
- Transformation: resources
Step One: Planning
- The Digital Switchover is happening now, with the final deadline in 2025, when the analogue networks will be switched off. You need to assess the overall impact upon your organisation and care services
- With changing demographics and increasing uptake, the numbers of digital care technology service users are expected to double by 2041
- Digital care technology is capable of a wider range of functionality which opens an opportunity for a broader service to users, better use of data, interoperability between equipment and prevention of future ill-health
- Digital technology is more expensive than analogue, and likely to require refresh more often, so ongoing increased upgrade costs need to be considered
- Adapting procurement approaches to focus more on quality than lowest cost may offer better outcomes and higher long-term tangible savings; here’s a recent procurement guide describing a range of approaches. This can increase benefits through preventing crises and escalation of care needs, but requires workforce redesign and culture change alongside technology.
- The opportunity to gather and use data from digital solutions is the key difference. Data can increase the focus on prevention, increase personalised care assessment and planning, inform social care commissioning and drive continuous improvement of the service. These are all sources of value for councils. See the Case Studies for more details.
- Some existing and new providers may falter in their plans to address the digital switchover, and you need to be prepared to change or support providers through this process
Planning: Resources
Switchover Readiness Assessment Tool
There are just 6 key questions which should take just a few minutes to answer. Each question scores from 1-5 points
- Use the tool to assess how well your council has planned for the upcoming Digital Switchover
- If the answers do not quite match your situation, choose the one that fits the best
- At the end, calculate your score and see what else you might need to be doing to ensure a successful switchover
Scoring and assessment
- Add up your total score from questions 1-6. You should then have a score out of 30.
- Assess yourselves according to the following table
- Score 6-12: The 2025 deadline is approaching fast, and you need to start planning now how you will safely support service users and suppliers through the switchover process
- Score 13-18: You’ve already made some steps to ensure a safe switchover, but there are key areas which may need more attention, and there’s still the opportunity to move further, faster
- Score 19-24: Congratulations, you’ve already got most of the building blocks in place to switch over to digital, in a way that will support service users and suppliers along the way
- Score 25-30: Wow, all the elements are in place for a successful transformation of digital care technology services in your area, with long term benefits and cost savings lined up
Step Two: Switchover
- The switchover will be completed by care technology suppliers, but this activity needs to be centred around the service users’ needs.
- This process has several potential challenges that need to be overcome; for example, contracts may be expiring or renewing anyway. However, alongside this are opportunities to enhance the service provided and improve outcomes.
- In the over 75 cohort, a robust telecare system provides benefits of reduced social care support, hospital bed days, ambulance call outs and home care visits. Scotland has estimated that digital care technology led to £99 million per annum benefit to the local health partnership from a £39 million spend.
- Scotland have already run a switchover program which has provided wide-ranging material that can be useful to commissioners in England.
Switchover Checklist
The following is a simple checklist you can use to ensure all key considerations are covered and considered for the digital switchover
- Switchover Costs: budget for switchover only: Scottish experience was > £188 per service user
- Communications Supplier Plans: consider suppliers’ digital rollout to exchanges in your area
- Care Technology Suppliers:
- Plans: contact equipment suppliers to check their plans and progress
- Contracts: see what is included (if anything) for switchover or upgrades (new functionality)
- Contracts: prepare business cases to secure funding for new services
- Contracts: procure switchover services and digital care technology from existing or new suppliers to ensure continuity
- Ongoing costs: Negotiate and agree connectivity and ongoing service costs for digital tech
- Service users: Consider how they and their families and carers are adequately supported and communicated with during and after the switchover
- Digital inclusion: In particular, ensure that plans consider how to include everyone in the switchover activities and immediately afterwards
- Staff and partners: Communicate with social care staff and partner providers so that they can consider the impact of the changes upon their services; involve them and their service users – they will be key to identifying vulnerable people and supporting them through the changes.
- Governance and risk: This key project requires tracking and reporting back to commissioners and leadership, and the associated risks need to appear at a corporate level given their potential seriousness.
Switchover: Resources
Step Three: Transformation
- The minimum pathway through the digital switchover is to simply replace the current analogue systems with digital equivalents. However, this brings with it challenges and would result in at best the same service offered most likely at an increased cost; so, an investment for the council with no obvious return.
- A switch to digital brings additional costs compared with analogue services; in particular the need to connect to an IP address. This leads to initial costs of £200-260 per device (with a 12-month SIM card) and then over £5 every month per SIM afterwards.
- There is opportunity to enhance the service provided by incorporating other digital care technology and making use of new data sources that would result in improved service for the users, and potentially lower other care costs. Our Case Studies show different ways that this might be achieved.
- It is important to move rapidly on this to ensure that the deadline is met for all users, and nobody is left without provision. There is a great potential to enhance the care provided but it needs to be alongside a programme that meets the key deadlines.
Transformation: making the business case
Potential benefits from moving to digital care technology, facilitated by service design and partnership working with housing, health, social care and industry partners:
- A shift towards a more preventative approach to care and support facilitated by next generation technology and data
- An opportunity to develop self-service models for installation of new technologies (plug and go)
- Improved workforce capacity and flexibility e.g., through virtual care visits
- Self-purchase / consumer technologies can be linked in with commissioned technologies to reduce costs and create a personalised technology offer
- Automated reporting on complex data, that would support greater personalisation of services for an individual person, a data driven approach to care assessment and planning, and to inform commissioning
- Integration of telecare within the broader health & social care system, to enable a shift to more proactive, predictive and preventative models
Some of these benefits will reduce the costs of running the service; more significant gains can be made by preventing, reducing or delaying the costs of care delivery. More content suggestions for a business case are given in the sections below.
Transformation- Case Studies
Case Study 1 - Gateshead Council
- An in-house traditional telecare offer with a monitoring and response centre
- Gateshead planned for the digital switchover to happen in line with their normal equipment renewal programme, over a 5 year period, now in year 4
- The new ARC has improved functionality, workflows and data capabilities
- Alarms were left until the later stages of the programme, and flexible procurement frameworks allow purchasing of a range of equipment to match exact needs
- Along the way, Gateshead have learnt many valuable lessons that will be useful to other councils embarking on their switchover journey
- They are now able to plan the next phase of their transformation, making more use of data and digital capabilities in the longer term
Read the full Gateshead Case Study
Case Study 2 - Suffolk
- A ‘big bang’ transformative approach through an extensive procurement process, with over 1000 referrals achieved in the first 9 months
- Gross savings of £2.2m from those first 1000 referrals
- Outcomes and satisfaction with the technology are high with residents, staff and families
- A great deal of effort was put into developing the skills and confidence of staff, partners, residents and families, as well as a widespread culture change programme